Laboratory Revenue Cycle Management: Choosing The Best One
This guide will show you how to optimize your daily lab operations. From the moment your staff enters an order to the final reimbursement.
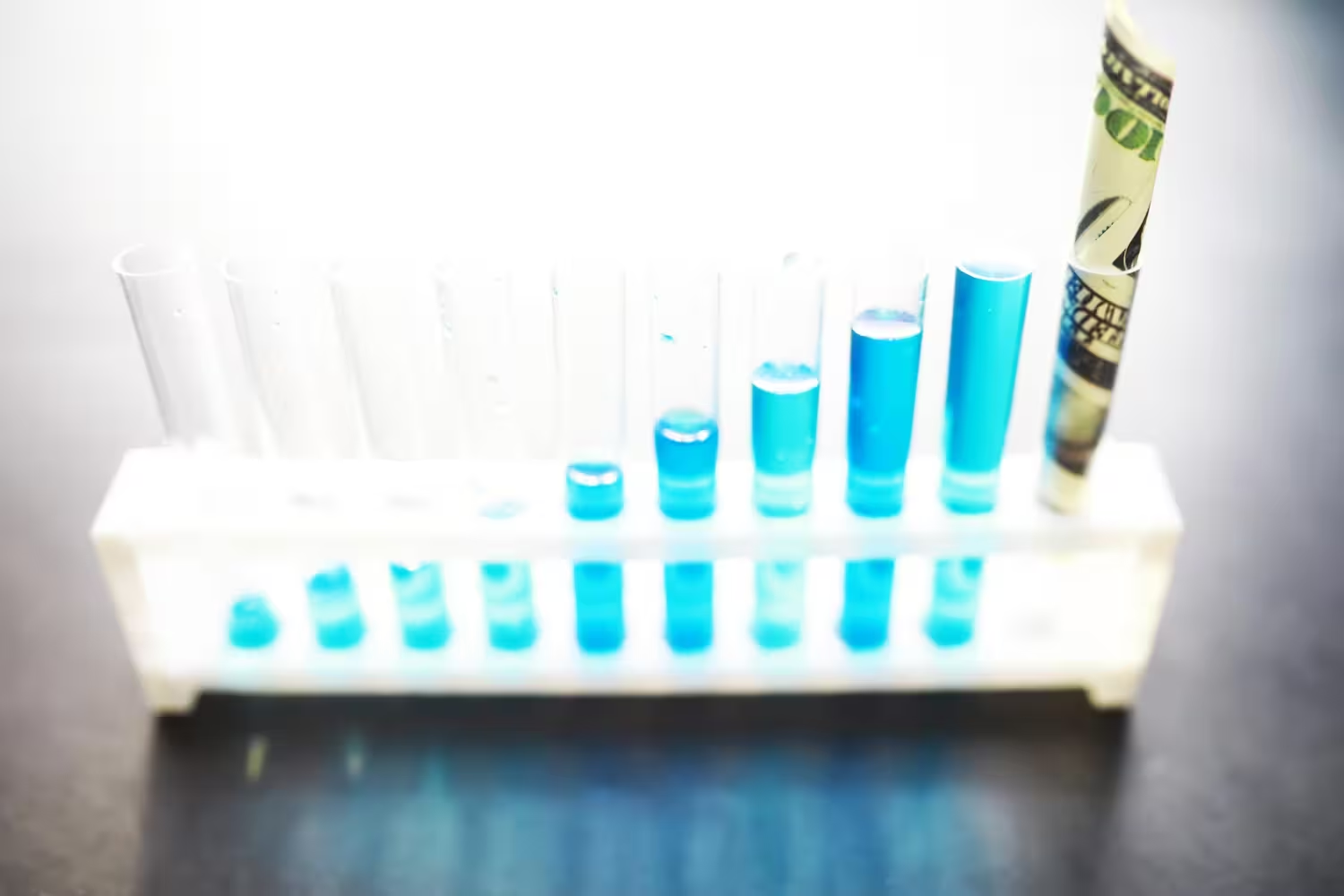
Did you know that 70% of medical decisions depend on laboratory results?
That statistic highlights just how essential laboratory services are to patient care. Keeping clinical lab processes running smoothly allows for faster diagnoses. It helps patients receive accurate treatment in a reasonable amount of time.
When it comes to a fast and accurate workflow, revenue cycle management solutions are key. With over 25 years of experience helping streamline revenue cycle management for labs, trust me when I say that the last thing you is a slow, outdated RCM process.
Revenue cycle management is the blueprint that maps out a patient's healthcare journey. It starts from the moment they make an appointment until the bill gets paid. Medical laboratories are no different. They need to be aware of their RCM lifecycle just like private practices or hospitals. Keeping a close eye on claims is essential to ensure tests get coded correctly and sent out on time.
Lately, labs are feeling the pressure. They’re handling more tests than ever. All while insurance companies keep changing the rules. This obviously makes it a struggle to keep cash flow steady. To stay ahead, labs can't just sit back and wait for billing problems to pop up. They need a proactive RCM strategy that catches errors before they happen. This guide will show you how to optimize your daily lab operations. From the moment your staff enters an order to the final reimbursement.
What is Laboratory Revenue Cycle Management?
Laboratory revenue cycle management (Lab RCM) is an end-to-end financial and administrative process. It manages claims submission and payment collection for diagnostic services. Unlike physician billing, laboratory billing involves a high volume of smaller claims. As well as highly specific coding requirements for pathology, molecular, and clinical testing. So it can be a little more intense, to say the least.
Being able to manage this cycle ensures that clinical laboratories get paid promptly. This reduces the risk of revenue leakage and inaccuracies. Ensuring the lab has the capital to provide top-tier patient care.

It also helps labs:
- Maintain compliance.
- Improve operational efficiency.
- Respond quickly to billing challenges.
The unique complexities associated with laboratory revenue cycle management further emphasize the importance of partnering with the right RCM software (like Etactics). More on this later.
The Seven Stages of the Laboratory Billing Process
Like I mentioned, laboratory billing processes can be a bit tricky. With all its nuances, some billers and coders might struggle making ends meet. Without revenue cycle management software, small details can fall through the cracks.

Here are the seven steps of the laboratory billing process:
- Collection: Gathering accurate patient demographics and insurance information. This usually happens at the point of test order creation. Incomplete or incorrect data is one of the leading causes of denials later on.
- Verification: Use an RCM system to confirm coverage, eligibility, and Medicare status. Doing this before testing begins helps to prevent front-end denials.
- Coding: Assigning accurate CPT and ICD codes is a major part of any revenue cycle operation. This stage is where coding errors most frequently lead to delays. Especially as new tests emerge and coding guidelines change.
- Claim Submission: Send scrubbed claims to the payer. This step ensures compliance with payer-specific rules.
- Payment Collection: Reconciling payments against accounts receivable. Also, managing patient billing for remaining balances. These are becoming more common with high-deductible health plans.
- Denial Management: Identifying why denied claims occurred. Analyzing root causes and executing a strategic appeal process. Instead of simply reworking claims.
- Analysis and Reporting: Using analytics and data management to check performance. All while continuing to improve outcomes.
Key Metrics Every Laboratory Should Monitor
When it comes to having a strong laboratory RCM strategy, you need to have the data to back it up. Tracking the right key performance indicators (KPIs) allows labs to identify inefficiencies sooner. This way, billing teams can take proactive action.

Here are a few basic KPIs every effective laboratory billing team should know:
- Clean Claim Rate: Measures how many claims your team submits without errors. A rate above 95% indicates efficient billing processes. By the way, labs that use Etactics maintain a 98% clean claim rate year over year!
- Days in Accounts Receivable: Tracks how long it takes to collect payment. Lower days in AR improve cash flow and signal faster reimbursement cycles.
- Denial Rate: Shows the percentage of claims rejected by payers. Keeping this below 5% is critical for financial stability.
- Patient Collection Rate: Measures how effectively billing teams collect patient balances. This is increasingly important as patient responsibility rises.
- Revenue Leakage: Identifies gaps between expected and actual revenue. These gaps are often due to underpayments, missed charges, or inefficiencies.
- Turnaround Time: Tracks how quickly claims move from submission to payment. This directly impacts cash flow consistency.
Monitoring these KPIs gives laboratories the visibility needed to make faster decisions. Also, it helps reduce revenue loss and improve overall performance!
Key Benefits of Modern Lab RCM Software
Manual billing processes can no longer keep up with the complexity of modern diagnostics. As testing volumes grow and payer requirements change, relying on outdated workflows leads to delays. As well as errors and missed revenue opportunities. This is where specialized laboratory revenue cycle management software comes in.
By reducing the need for manual data entry, these solutions lower the risk of human error. Reducing the likelihood of rejected claims and costly rework.

Automation streamlines key steps like:
- Eligibility verification.
- Claims scrubbing.
- Submission.
This helps speed up reimbursement and maintain a steady cash flow. Preventing errors before submitting claims leads to fewer denials.
Modern RCM platforms help laboratories stay compliant with constantly changing payer rules. They also offer real-time analytics through dashboards and reporting tools. Giving teams visibility into performance trends and allowing them to make better decisions.
Etactics helps laboratories with all of those automation capabilities on the RCM day-to-day side. In other words, we help your lab crush through and streamline financial bottlenecks that may be leading to slower revenue growth. Meanwhile, our Business Intelligence (RevVitals) platform gives you real-time insight on how your organization’s RCM is performing.
How to Automate Lab Revenue Cycle Management
The healthcare industry is digitizing rapidly. Payers are already using AI to flag claims. To stay competitive, labs must automate where it matters most.
By integrating RCM software directly with your laboratory information system, you can:
- Trigger real-time insurance discovery.
- Automate claims workflows.
- Reduce manual intervention.
- Flag errors before submission.
- Predict denials.
- Streamline follow-ups.
Automation doesn't just improve speed. It improves accuracy and reduces administrative headaches.
Why Advanced Laboratory Billing Solutions are Essential
Billing solutions must now evolve enough to handle complex lab testing requirements.
Advanced platforms provide the transparency needed to identify bottlenecks. Plus, check performance and optimize workflows.
Without this visibility, labs risk falling behind on payer-specific requirements. This can lead to higher denial rates, compliance risks, and inconsistent cash flow.
Overcoming Common Revenue Cycle Management Challenges
Laboratories today face several persistent revenue cycle challenges. All which significantly impact financial performance. One of the most common issues is high denial rates. These are often caused by coding errors, missing documentation, or outdated payer requirements.
Laboratories now benefit more from using analytics to identify patterns. As opposed to addressing denials one-by-one. This strategy allows your team to resolve root causes proactively.
Lab billing teams also often face fragmented billing processes as a whole. This is due to laboratories typically working with multiple payers. Each payer has their own rules and submission requirements. This adds layers of complexity. It also increases the likelihood of errors throughout the billing cycle. Many labs still rely heavily on manual workflows. Which can slow down operations and make mistakes more likely. Especially as claim volumes continue to rise.
Regulatory compliance is another concern for labs. They must check and update their processes to remain compliant with healthcare regulations.
Rising patient financial responsibility has also made collecting payments more difficult. Higher patient balances require more effective engagement strategies. Also, clearer communication and flexible payment options to ensure successful collections.
Should You Outsource or Use In-House Billing Services?
Whether to outsource to billing services or keep your process in-house depends on you. Here are some things to consider:
- In-House: This path offers full control and data visibility. It does require an investment in RCM software and specialized staff.
- Outsourced Services: Provides immediate access to billing and reimbursement expertise. Also, reduces administrative burden. You may have less direct control over daily tasks.
- Hybrid: Many effective labs keep core functions in-house while outsourcing specialized tasks. Such as complex pathology appeals.
Best Practices for Better Reimbursement
Many laboratories are now turning to revenue cycle management experts and advanced platforms. Not only to improve performance, but also stay ahead of growing financial challenges. These solutions combine technology with industry expertise. Helping labs shift from a reactive billing process to a more proactive and accelerated one.
To maximize revenue and reduce bad debt, laboratories should focus on:
- Check performance regularly and adjust strategies based on KPI insights.
- Focus on clean claims to avoid costly rework and reduce denials.
- Leverage automation and analytics to catch errors early.
- Integrate systems to cut data silos and improve accuracy.
- Stay proactive with compliance and evolving payer requirements.
By taking this approach, labs can strengthen their day-to-day workflow. Facilitating better financial stability, improved efficiency, and ensuring long-term success. Even in an increasingly complex healthcare environment.
Emphasize your product's unique features or benefits to differentiate it from competitors
In nec dictum adipiscing pharetra enim etiam scelerisque dolor purus ipsum egestas cursus vulputate arcu egestas ut eu sed mollis consectetur mattis pharetra curabitur et maecenas in mattis fames consectetur ipsum quis risus mauris aliquam ornare nisl purus at ipsum nulla accumsan consectetur vestibulum suspendisse aliquam condimentum scelerisque lacinia pellentesque vestibulum condimentum turpis ligula pharetra dictum sapien facilisis sapien at sagittis et cursus congue.
- Pharetra curabitur et maecenas in mattis fames consectetur ipsum quis risus.
- Justo urna nisi auctor consequat consectetur dolor lectus blandit.
- Eget egestas volutpat lacinia vestibulum vitae mattis hendrerit.
- Ornare elit odio tellus orci bibendum dictum id sem congue enim amet diam.
Incorporate statistics or specific numbers to highlight the effectiveness or popularity of your offering
Convallis pellentesque ullamcorper sapien sed tristique fermentum proin amet quam tincidunt feugiat vitae neque quisque odio ut pellentesque ac mauris eget lectus. Pretium arcu turpis lacus sapien sit at eu sapien duis magna nunc nibh nam non ut nibh ultrices ultrices elementum egestas enim nisl sed cursus pellentesque sit dignissim enim euismod sit et convallis sed pelis viverra quam at nisl sit pharetra enim nisl nec vestibulum posuere in volutpat sed blandit neque risus.
Use time-sensitive language to encourage immediate action, such as "Limited Time Offer
Feugiat vitae neque quisque odio ut pellentesque ac mauris eget lectus. Pretium arcu turpis lacus sapien sit at eu sapien duis magna nunc nibh nam non ut nibh ultrices ultrices elementum egestas enim nisl sed cursus pellentesque sit dignissim enim euismod sit et convallis sed pelis viverra quam at nisl sit pharetra enim nisl nec vestibulum posuere in volutpat sed blandit neque risus.
- Pharetra curabitur et maecenas in mattis fames consectetur ipsum quis risus.
- Justo urna nisi auctor consequat consectetur dolor lectus blandit.
- Eget egestas volutpat lacinia vestibulum vitae mattis hendrerit.
- Ornare elit odio tellus orci bibendum dictum id sem congue enim amet diam.
Address customer pain points directly by showing how your product solves their problems
Feugiat vitae neque quisque odio ut pellentesque ac mauris eget lectus. Pretium arcu turpis lacus sapien sit at eu sapien duis magna nunc nibh nam non ut nibh ultrices ultrices elementum egestas enim nisl sed cursus pellentesque sit dignissim enim euismod sit et convallis sed pelis viverra quam at nisl sit pharetra enim nisl nec vestibulum posuere in volutpat sed blandit neque risus.
Vel etiam vel amet aenean eget in habitasse nunc duis tellus sem turpis risus aliquam ac volutpat tellus eu faucibus ullamcorper.
Tailor titles to your ideal customer segment using phrases like "Designed for Busy Professionals
Sed pretium id nibh id sit felis vitae volutpat volutpat adipiscing at sodales neque lectus mi phasellus commodo at elit suspendisse ornare faucibus lectus purus viverra in nec aliquet commodo et sed sed nisi tempor mi pellentesque arcu viverra pretium duis enim vulputate dignissim etiam ultrices vitae neque urna proin nibh diam turpis augue lacus.



